Breast cancer is the most common cancer diagnosed in the UK with around 55,000 new cases a year. There are a variety of symptoms which it is important to look out for and get checked out if you have any concerns.
Read on to find out more about it. However, this is no substitute for medical advice, so if you think you may have breast cancer, it is important that you see your GP as the first point of call to get a diagnosis and, if you do have breast cancer, to talk through the possible treatments with a specialist and find the right solution for you.
What is breast cancer?
Breast cancer accounts for around 15 per cent of newly diagnosed cancers in the UK. This makes it the most common one. It’s a condition that affects the breast tissue and develops when abnormal cells grow and divide and form a tumour. It most often starts in the cells that line the milk ducts. Most people who get it are women, but it can affect men too.
What causes breast cancer?
There are a number of circumstances that can put you at greater risk of breast cancer.
If you have had breast cancer before you are at higher risk of getting it again, and if you’ve had a non-cancerous breast lump previously, then, depending on the type, you may be at higher risk of developing breast cancer.
Certain circumstances beyond your control are risk factors and these include your age – as the risk increases the older you are. NHS figures show that about eight in every 10 cases of breast cancer affect women aged over 50.
Does a family history of breast cancer mean I will get it?
A family history of breast cancer or ovarian cancer may mean that you are at higher risk of getting breast cancer, but not necessarily. Most often cases of breast cancer are not thought to be genetic, but the BRCA1 and BRCA2 genes can increase the risks of getting breast cancer and ovarian cancer.
However, according to Cancer Research UK only two per cent of breast cancers are linked to changes in these genes, so they are not common.
Women who have been through menopause and are obese or overweight may have a greater risk too. This may be caused by the amount of oestrogen produced.
Hormone Replacement Therapy (HRT) has been linked in the past to breast cancer, though taking vaginal oestrogen is not thought to be a risk factor. Risks from HRT depend on many variables so it is important to talk to your GP about it to work out what is best for you in the light of your own individual circumstances.
Other factors that increase risk
Exposure to oestrogen can be a cause, so if you menstruate for a longer time, i.e. if you started early and then have a late menopause, the risk may increase slightly.
There is a small increase in risk for those who take the contraceptive pill, though the risk goes down after you stop taking it and returns to normal levels 10 years after you stop taking the pill.
Drinking alcohol is a risk factor and the risk increases the more of it you drink.
Cancer Research UK say that being inactive brings with it a small increase in breast cancer risk, and they say that doing less than two-and-a-half hours of exercise a week puts you into that category.
Breast cancer symptoms
There are a number of symptoms of breast cancer and if you find any of these they must be checked.
For many women, the first thing they may notice is a lump. The NHS website notes that most breast lumps are not cancerous, however, it is vital to get any lump checked out.
Changes in shape or size or feel – this could happen to just one breast or to both of them.
Your nipples can display symptoms. For example, the appearance of them can change, so they may appear sunken into the breast or turn in. Another symptom is discharge from your nipples. This fluid can have blood in it. A rash on or around the nipples or dimpling or puckering of the breasts are other symptoms to look out for.
Checking yourself for signs of breast cancer should also include your armpits, as a lump or swelling or thickening there is another possible symptom.
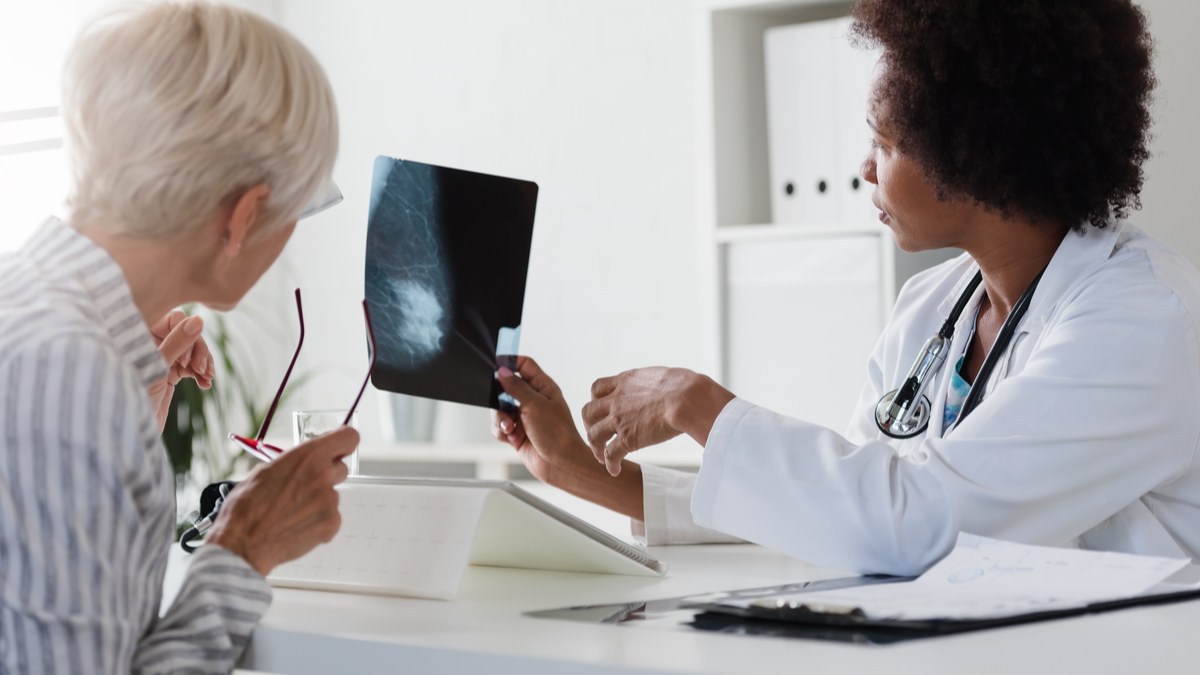 Breast cancer diagnosis
Breast cancer diagnosis
If you notice any of the symptoms of breast cancer or any changes to your breasts it’s important to see your GP, so you can be examined.
You will be referred to a specialist breast unit where you can have a mammogram and possibly an ultrasound scan. These scans produce images that can show abnormalities.
Breast cancer may also be diagnosed through routine breast screening. Regular screening is offered every three years between the ages of 50 and 71.
Having a mammogram
This screening is done via a mammogram, which can allow specialists to spot tiny cancers that would not be detected from observing or feeling the breast.
Cancers can be picked up much earlier this way, usually making them easier to treat.
Around one in every 25 women screened will be called back for further checks, perhaps because the original mammogram was not clear enough.
Most will be fine, but one in four of those called back will be diagnosed with breast cancer. The screening service actually finds around nine cancers in every 1,000 who are screened.
What happens if cancer is suspected after screening?
If cancer is suspected a biopsy can find out more. This allows a sample of cells to be tested to see if they are cancerous. Most often this is done by using a needle to take a sample of tissue.
This may be done alongside an ultrasound, X-ray or MRI scan for extra precision.
If breast cancer is diagnosed there will then be other tests to find out what stage it is at and what grade of cancer it is.
What do the different stages mean?
The different stages, from stage 0 to stage 4 refer to a number of factors. These include the size, whether the lymph nodes are affected and whether it has spread. Stage 4 can be a tumour of any size, but it has spread to other parts of the body and this is called metastasis.
Other tests are carried out so that the doctors can get a fuller picture. This helps them plan what type of treatment is needed.
Breast cancer treatments
There are a range of medical treatments for breast cancer. A number of factors need to be considered including your general health, and whether you have been through the menopause. Other factors include how large the cancer is and, if it has spread, how far it has gone. Here are some of the most common:
Surgery
Surgery could involve the removal of the tumour, which is known as breast-conserving surgery. This can range from a lumpectomy to a surgery where a tumour and some surrounding breast tissue is removed. This may be followed up with radiotherapy. Alternatively, a mastectomy may be given, which is the complete removal of the breast. Breast reconstruction can be carried out. This may be done at the same time as the mastectomy, or later on.
Radiotherapy
There are a range of types of radiotherapy. The type used will depend on what sort of breast cancer you have and the type of surgery. It may be used to target the whole of the breast tissue that remains, to the chest wall, to the area where the cancer was taken from, or to the lymph nodes. Side effects can include fatigue, skin irritation and fluid building up in your arm.
Chemotherapy
Chemotherapy is used to destroy cancer cells. This may be carried out after surgery to target cells that were not removed, or sometimes it is used before surgery to reduce the size of a tumour. Chemotherapy is generally carried out as an outpatient every two to four weeks. It is given via a drip. Side effects include sickness, hair loss, tiredness, infections and a sore mouth. Some side effects can be eased with other medication.
Hormone treatment
Hormone therapy may be given depending on what stage, grade and type of cancer is being treated.
How to prevent breast cancer
It is not yet known whether it is possible to absolutely prevent it. The causes are not fully understood yet.
However, according to Cancer Research UK there are some things that may help reduce the risk including being physically active, limiting your alcohol intake and eating healthily.
Those women who definitely have a genetic risk of developing breast cancer can receive treatment to help prevent it. This may involve having a mastectomy or taking medication.







