In partnership with Healthspan
High cholesterol has no warning signs. No pain. No obvious symptoms. Yet it remains one of the biggest risk factors for heart disease in the UK, particularly in midlife when hormonal shifts quietly increase cardiovascular risk.
You can look healthy and feel well and still have raised cholesterol levels. That is what makes it so dangerous.
What High Cholesterol Actually Does
Dr Martin Lowe, Consultant Cardiologist at The Harley Street Clinic and The Portland Hospital, part of HCA Healthcare UK, explains:
‘While we find that all patients understand that having high cholesterol is bad, and has a negative effect on the cardiovascular system, it can be difficult for them to understand exactly what it is.
‘Once we have too much cholesterol in our body, these fatty substances can grow and make it difficult for blood to flow. In severe cases, this can cause a heart attack or stroke.’
LDL cholesterol builds up inside artery walls, narrowing them and increasing the risk of heart attack and stroke.
Why Midlife Increases Risk
Cholesterol levels are influenced by age, hormones and fat distribution.
After menopause, oestrogen declines. As this protective hormone falls, non-HDL cholesterol often rises and HDL may drop.
At the same time, abdominal fat becomes more common, and this type of fat is more strongly linked to cardiovascular risk.
You Can’t Feel High Cholesterol
Rob Hobson, Registered Nutritionist working with Healthspan, says:
‘You cannot tell if you have high cholesterol based on symptoms alone. High cholesterol doesn’t present with noticeable signs or symptoms in the early stages. Instead, high cholesterol is typically determined through a blood test.’
High cholesterol is often called a ‘silent’ condition because there are no obvious warning signs.
Dr Tina Ghela, Digital Clinician at Medichecks, adds, “High cholesterol doesn’t always have visible symptoms or affect how you look or feel, which is why it’s often called a “silent” condition. Most people with high cholesterol don’t feel any different. You can be thin, active, and feel healthy — and still have high LDL (“bad”) cholesterol. Genetics can also play a role. Familial hypercholesterolemia (FH) is a genetic condition that causes high cholesterol even in people who eat well and exercise. This is why regular screening matters; regular blood tests are essential.”
TV doctor Dr Hilary Jones who works with Healthspan explains, “High cholesterol doesn’t always go hand in hand with how you look or feel. Even people who are slim, active, and appear healthy can have raised levels – and often they won’t know unless they get tested. That’s why regular checks in your 40s and 50s are so important.”
Could Plant Sterols Help Lower Your Cholesterol?
In short, yes, particularly when combined with dietary changes.
Plant sterols are naturally occurring compounds that reduce the absorption of cholesterol in the gut, lowering circulating LDL levels.
Research shows that a daily intake of 2.4g can reduce LDL cholesterol by up to 12.5 per cent within two to three weeks when taken alongside a heart-healthy diet.
That reduction may sound modest, but even small decreases in LDL are linked to meaningful reductions in cardiovascular risk over time.

Try Healthspan Plant Sterols Supplements
Healthspan Plant Sterols Supplements, (800mg, £21.99, suitable for vegan and vegetarians, healthspan.co.uk) are designed to deliver an effective daily dose and are taken with meals, typically one tablet three times a day, to support LDL reduction as part of a broader heart health strategy. If you are looking to maintain levels, then just taking one a day can support alongside diet and lifestyle choices.
Rob explains, “Statins and plant sterols are often compared, but they work in very different ways and can complement each other. Statins block an enzyme in the liver that helps produce cholesterol, which makes them very effective at lowering LDL levels and reducing the risk of heart attacks and strokes. They’re especially important for people with very high cholesterol or those at greater cardiovascular risk.
Plant sterols, on the other hand, are naturally occurring compounds that block cholesterol absorption in the gut. They can be helpful for people with more moderate elevations, or as an additional step for those already taking statins, where studies suggest they may have an additive benefit.
The decision isn’t so much an ‘either/or’ as statins are essential for many people, but diet, lifestyle, and supplements like plant sterols provide the foundation. For most people, it’s about combining the right medical treatment with everyday habits that support long-term heart health.’

Diet Does Matter
Diet has been consistently shown to play a central role in managing cholesterol levels. In fact, certain foods can help to actively lower LDL when eaten regularly.
Soluble fibre lowers cholesterol by binding to it in the gut. Oats, beans, lentils, fruit, especially apples, grapes and berries rich in pectin, along with seeds and vegetables, are easy ways to increase intake.
Plant-based proteins such as tofu, tempeh and legumes provide both fibre and protein, while healthy fats from nuts, seeds and extra virgin olive oil support overall heart health.
Switching to soya milk may also help thanks to its isoflavones and protein content.
And fibre only works effectively when fluid intake is adequate, so hydration matters too.
The Bottom Line
High cholesterol rarely announces itself.
The only way to know your levels is through a blood test, particularly from midlife onwards. So, keep an eye on your cholesterol levels and blood pressure.
If levels are raised, diet and lifestyle form the foundation. For some, evidence-based options such as plant sterols may provide additional support in lowering LDL cholesterol.
High cholesterol may be silent, but it does not have to go unchecked.
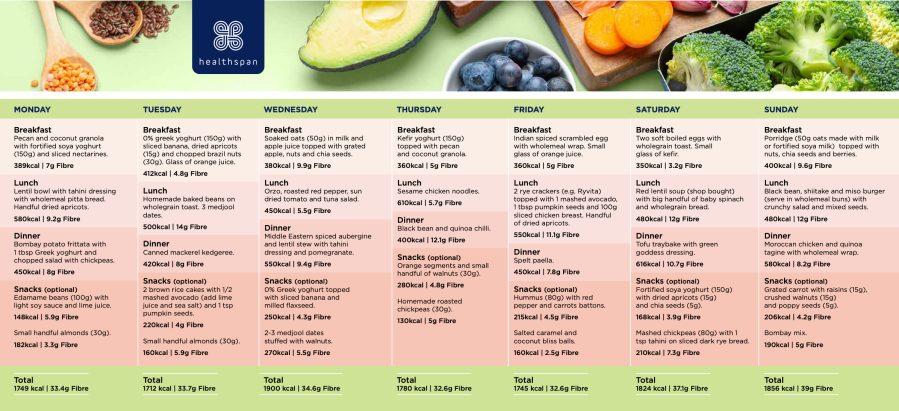
Visit Rob Hobson’s Cholesterol Lowering Meal Planner at Healthspan